Headaches often get blamed on dehydration, stress, or a poor night's sleep. Yet growing medical research points to another factor that rarely receives attention: body weight. Several large studies now suggest that obesity may increase the chances of frequent headaches and migraines, especially among women under 50.
Health data involving more than 200,000 women indicates that individuals with obesity face a significantly higher likelihood of experiencing severe headaches. Compared with people who maintain a healthy body mass index (BMI), the risk of frequent headaches may rise by as much as 80 percent.
Neurologists say this link deserves more attention because the biological connection between excess weight and headaches is becoming clearer. According to Dr. Amrut SD, Consultant Neurologist at Manipal Hospital, Goa, obesity is often ignored when doctors evaluate chronic headache disorders.
“Headaches are not always caused by stress or dehydration. Obesity is a significant, yet frequently overlooked, risk factor for severe, chronic, and recurrent headaches. In some cases, they can become debilitating and even affect vision,” says Dr. Amrut.
Understanding why this happens may help many patients manage headaches more effectively while improving overall health.
Why Obesity Can Trigger Headaches
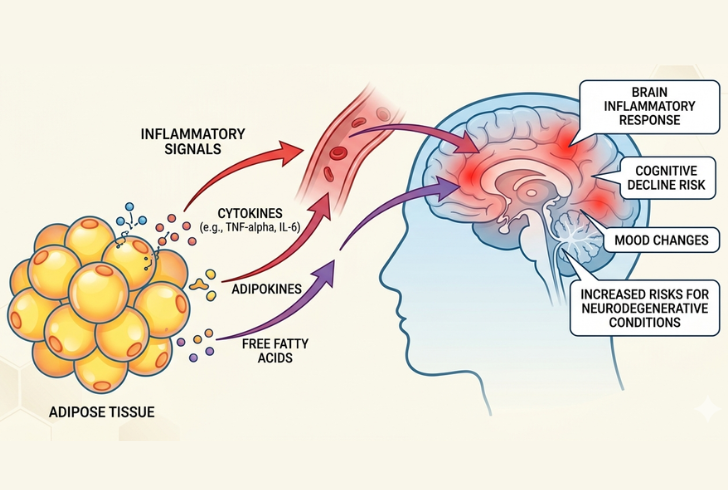
Gemini AI | Adipose tissue acts as a gland, releasing inflammatory chemicals like CGRP that trigger migraines.
Scientists believe the link between obesity and headaches begins with inflammation inside the body. Fat tissue does more than store energy. It also behaves like a hormone-producing gland.
According to Dr. Amrut, adipose tissue releases inflammatory chemicals that can influence how the nervous system processes pain.
“Fat tissue, known as adipose tissue, is metabolically active and behaves like a gland. It produces pro-inflammatory chemicals such as calcitonin gene-related peptide (CGRP), which is known to trigger migraine pain,” Dr. Amrut explains.
These inflammatory compounds can increase sensitivity within the brain’s pain pathways. As a result, the nervous system becomes more reactive, making migraine attacks more likely.
Medical research supports this explanation. Population studies consistently show that individuals with higher BMI levels report more migraine attacks than those with healthy weight levels. The relationship appears strongest among adults younger than 50.
When Occasional Headaches Turn Chronic
Weight-related inflammation may also influence the frequency of headaches. In some cases, an occasional headache can develop into a long-term condition.
Dr. Amrut notes that people living with obesity may be 40 to 80 percent more likely to experience migraines compared with individuals of normal weight.
An increasing BMI can also convert episodic migraines into chronic daily headaches, which doctors define as headaches occurring more than 15 days per month.
Once headaches reach this stage, treatment often becomes more complicated.
“Standard medications may not always provide full relief. Some patients require specialised therapies such as topiramate, greater occipital nerve (GON) blocks, or botulinum toxin injections, along with strict lifestyle modifications including at least 15% weight reduction,” Dr. Amrut says.
These treatments aim to control nerve activity, reduce inflammation, and prevent recurring migraine attacks.
A Serious Condition Linked to Obesity
In certain cases, persistent headaches related to obesity may signal a rare neurological disorder known as Idiopathic Intracranial Hypertension (IIH).
This condition occurs when pressure inside the skull rises without a clear medical cause. Research shows that more than 90 percent of people diagnosed with IIH are overweight or obese, particularly women of reproductive age.
Dr. Amrut explains that the condition should never be ignored because it may affect eyesight.
“Idiopathic intracranial hypertension is a severe headache disorder caused by increased pressure inside the skull. It is strongly linked to significant weight gain and can sometimes lead to permanent vision loss if not treated in time,” he says.
Increased pressure around the brain can compress the optic nerve, which carries visual signals to the brain. Without timely treatment, long-term damage may occur.
Signs That Require Medical Attention

Freepik | Seek immediate medical care for any sudden, significant changes in your headache patterns.
Some headache symptoms may indicate IIH or another serious neurological issue. Doctors recommend prompt medical evaluation if any of the following signs appear:
- Sudden change in headache pattern
- Headaches that worsen while lying down
- Blurred or gradually worsening vision
- Buzzing or ringing sounds in the ears
- Headaches that do not respond to common medications
Dr. Amrut warns that vision problems can develop if the condition remains untreated.
“Patients with IIH may have a high risk of losing vision if the condition is not treated. In some cases, surgery may be needed to relieve pressure on the optic nerve,” he explains.
Diagnosis usually involves several medical tests, including detailed eye examinations, brain imaging scans such as MRI, and measuring cerebrospinal fluid pressure through a lumbar puncture.
These tests help doctors confirm whether elevated pressure inside the skull is responsible for the symptoms.
Can Weight Loss Reduce Headaches?
Encouragingly, medical research suggests that weight loss may help reduce headache frequency and intensity.
“Being overweight is a modifiable risk factor. Many patients notice fewer and less severe headache attacks after losing weight,” says Dr. Amrut.
Studies focusing on patients with idiopathic intracranial hypertension show that losing 6 to 10 percent of body weight may significantly improve symptoms. In some cases, the condition may even go into remission.
Weight reduction may help ease headaches by lowering inflammation in the body, improving metabolic health, reducing pressure on brain structures, and supporting better hormonal balance.
For migraine sufferers, even modest weight loss may reduce how often attacks occur.

Freepik | diana.grytsku | Losing weight can significantly reduce headaches by improving inflammation, metabolism, and hormonal balance.
Lifestyle Changes That Support Relief
Doctors often encourage a gradual approach to lifestyle changes. Long-term results are more likely when habits are sustainable and consistent.
1. Balanced nutrition
Nutrient-dense meals can help regulate inflammation and energy. A focus on whole foods—vegetables, fruits, grains, and lean proteins—is key.
Limiting processed foods and sugar can also support metabolic health.
2. Regular physical activity
Exercise helps manage weight and improve circulation. It may also reduce inflammation linked to headaches.
3. Medical guidance
Professional support may be needed in some cases, including medications or structured programs.
4. Focused weight management
Dr. Amrut notes:
“Reducing excess weight can lead to fewer headache attacks…”
Persistent headaches may signal deeper issues. Addressing weight and lifestyle factors can help reduce symptoms and improve overall well-being.

